Defined by the Autism Society, Autism Acceptance month is about moving beyond awareness and promotes the celebration of neurodiversity. By honoring the lived experiences and identities of individuals with Autism, we can promote a community centered on inclusion, understanding, and support8.
As a neuro-affirming Registered Dietitian, implementing a person-centered approach when working with individuals with Intellectual and Developmental disabilities on their nutrition goals is essential to provide them with autonomy and confidence when making food and nutrition choices that align with each of their preferences and needs.
In this blog post, I hope to shed some much-needed light on some of the realities of autism and nutrition and empower families with the knowledge they need to nurture their loved ones’ wellbeing, one step (meal) at a time!
This article is available in ASL, scroll down to see video at the bottom of the page.

1. Food selectivity is not defiance
When either a child or adult with autism eats a limited range of foods, it’s usually not about defiance, lack of effort or even a poor appetite2. It’s often connected to:
- Sensory processing differences1 (texture, smell, temperature, sounds or even color)
- Need for predictability3
- Interoceptive differences (difficulty recognizing hunger/fullness)
- Anxiety or past food-related stress4
Food Sensitivity is often a nervous system strategy rather than a willful behavioral problem5.
2. There is no one “Autism” diet
It’s completely understandable that families look for solutions when a child or adult is struggling with GI discomfort, limited food variety, or daily stress around eating. Over time, various dietary approaches have been studied, promoted and elicited as potential “treatments” for autism.
For example, dietary interventions such as gluten-free/casein-free (GFCF) diets have been widely discussed in relation to autism. While some individuals have reported personal benefits from these specialized diets, the current research does not conclusively support their efficacy for the broader autism population7. While some individuals with autism may have co-occurring GI conditions, allergies, or medical needs that require specific dietary support, broad restrictive diets are not universally helpful and can sometimes increase stress or nutritional risk, particularly when implemented without professional supervision6.

That’s not to discount the real struggles and experiences of those who have found relief through these dietary changes, every person is unique and what works for one may not work for another. As a Registered Dietitian, my role is to provide evidenced-based nutrition guidance while acknowledging that there is still much to be learned about the complex relationship between autism and nutrition.
Nutrition can absolutely support health, energy, GI comfort and overall well-being, but it does not change someone’s neurotype. The goal is not to eliminate autism, it’s to help neurodivergent individuals thrive with food and help them eat in a way that feels safe, nourishing, and delicious! Working with a neuro-affirming registered dietitian provides person-centered autism and nutrition care including feeding strategies for Food Selectivity or Food Sensitivity.
3. Progress can appear in many forms
When it comes to a person wanting to work on food selectivity (FS) or Food Sensitivity (FS), progress isn’t always just adding “more foods”, It might look like
- Less anxiety during mealtime
- Tolerating a new food nearby (on the table or a neighboring plate)
- Expanding within a preferred food category
Adequacy and safety matter more than variety for variety’s sake.

4. Refrain from making food a “reward”
It’s common to see food as a motivator, especially in behavior-based settings. But when food becomes a reward or something to “earn” it can:
- Disconnect folks from hunger and fullness cues; When food becomes currency, internal cues can get overridden by external control10
- Increase pressure and anxiety around meals9
- Mixed messages: It can be confusing for individuals who are told to eat healthy for their well-being but simultaneously told that “treats” are rewards for positive behavior.
For individuals who have autism often navigate high levels of external demands, mealtimes can be one of the few spaces where autonomy and safety are preserved. With that said, in specific instances and settings, for example, during ABA (Applied Behavior Analysis) implementation and/or school settings, alternative rewards are preferrable, however minimal implementation of preferred snack or food in small quantities, if needed, is understandable in those settings.

5. Nutrition is one piece of the whole picture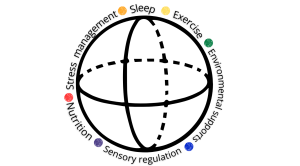
As a neuro-affirming registered dietitian I care deeply about the role that food plays in health. Adequate nutrition supports growth, energy, and overall well-being. At the same time, nutrition does not operate in isolation. Sleep, sensory regulation, movement, stress levels and environmental supports all play meaningful roles, particularly for neurodivergent individuals.
When families are navigating concerns around mood, focus, behavior, or energy, it’s important to look at the full picture rather than placing all expectations on food alone. Sustainable well-being comes from addressing multiple layers of support.
Interested in a particular nutrition topic/question covered in a future blog? Email nutritioncorner@jaynolan.org!
Access this article in ASL:
Medical Advice Disclaimer: The information provided on this blog is for informational and educational purposes only. No material provided in this blog, including images and graphics, is intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider before making any dietary changes or starting a new health care regimen. Do not neglect professional advice because of what you may have read in this blog.
References:
1. Cermak, S. A., Curtin, C., & Bandini, L. G. (2010). Food selectivity and sensory sensitivity in children with autism spectrum disorders. Journal of the American Dietetic Association, 110(2), 238–246. https://doi.org/10.1016/j.jada.2009.10.032
2. “Organization for Autism Research Grants.” Corporate Philanthropy Report, vol. 40, no. 2, Feb. 2025, pp. 16–16. DOI.org (Crossref), https://doi.org/10.1002/cprt.32205.
3. “Food Selectivity.” Association for Science in Autism Treatment, https://asatonline.org/research-treatment/clinical-corner/food-selectivity/.
4. “Easing Mealtime Stress.” Children’s Hospital of Philadelphia, 8 June 2020, https://www.research.chop.edu/car-autism-roadmap/easing-mealtime-stress#:~:text=Many%20children%20on%20the%20autism,food%20for%20these%20first%20tastes.
5. Riccio, M. P., Marino, M., Garotti, R., Tassiello, A., Maffettone, V., Pezone, M., & Bravaccio, C. (2025). Food selectivity in Autism Spectrum Disorder: implications of eating, sensory and behavioural profile. Frontiers in psychiatry, 16, 1587454. https://doi.org/10.3389/fpsyt.2025.1587454
6. Almohmadi N. H. (2024). Brain-gut-brain axis, nutrition, and autism spectrum disorders: a review. Translational pediatrics, 13(9), 1652–1670. https://doi.org/10.21037/tp-24-182
7. Önal, S., Sachadyn-Król, M., & Kostecka, M. (2023). A Review of the Nutritional Approach and the Role of Dietary Components in Children with Autism Spectrum Disorders in Light of the Latest Scientific Research. Nutrients, 15(23), 4852. https://doi.org/10.3390/nu15234852
8. Nebeker, Lindsey. “Autism Acceptance Month.” Autism Society, https://autismsociety.org/autism-acceptance-month/.
9. Fedewa, A. L., & Davis, M. C. (2015). How Food as a Reward Is Detrimental to Children’s Health, Learning, and Behavior. The Journal of school health, 85(9), 648–658. https://doi.org/10.1111/josh.12294
10. Bingeman, Brittany, and Jaqueline Neid-Avila. “Learning to Listen to Hunger and Fullness Cues.” Digital Commons Extension, Feb. 2018.



